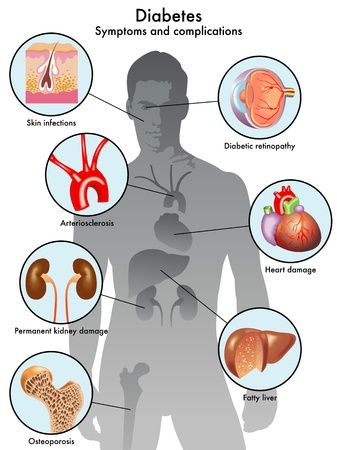
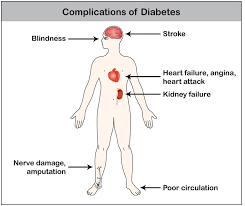
Knowing how to talk to someone struggling with a serious mental illness such as an eating disorder, or even an individual with just type 1 diabetes alone can be a minefield for family and friends. Both conditions are regarded as invisible illnesses that are often misunderstood. Innocent comments can quite easily be taken the wrong way entirely. My eating disorder will reframe and misconstrue anything it can potentially collude with and use against me. You somehow become psychic and can read minds. It’s often the case that I know I am being duped but I’ll gladly fall head first down that rabbit hole.
So that said, these are gentle suggestions of what not to say to someone with an eating disorder, type 1 diabetes or a comorbidity of the two. Mostly those flippant remarks that that can’t be caught until they are said out loud and then realisation hits. But sometimes it can be ignorance, it can be frustration and anger and shock tactics, none of which work but all of which are born from desperation.
I hope this might be of use to individuals in a supporting position for someone who is ill. Often the way our minds twist things can make absolutely no sense. These pointers are devised through not just my own experience but that of other eating disorder sufferers I know of, voices from some of my close friends, some that I have met in treatment settings, and also members of the diabulimia online Facebook community.
Please feel free to add any others you think are important via our social media pages and share this with your spouse, parents, siblings, your best friend or anyone you think might find them to be of use. My personal commentary is in bold
1. Try to avoid diet talk. Yes, sadly it’s normal. It’s messed up but it is inescapable. Women in coffee shops opting for skinny milk because they think they need to lose a few pounds or gaggles of young girls asking “do I look fat in this?” as they stand in front of the changing room mirrors. Gutting, but that is the reality of it. Still, making an effort not to talk directly about weight loss and diets to someone with an eating disorder is important. We have enough of that talk going on inside our heads to contend with. Especially don’t ask us for diet tips. Actually, this is never okay, to anyone, as you never know the reasons behind weight loss, or gain for that matter
2. Further to this, a bit of a difficult one that mostly applies in early recovery when an eating disorder sufferer is struggling to accept their body and the guilt that may come alongside eating and accepting insulin. “You look so much better/healthier/brighter/your face is so much fuller!” Okay so we might know these are intended as compliments, they show compassion and the fact that someone may be so relieved to see you looking better. But again, someone with an eating disorder can manipulate those words automatically. We might hear “You look fat”, “you must not be ill anymore.” I also know that these kinds of things can be said when actually someone is looking horrendous, as some kind of way to displace that awkwardness and reassure when someone appears to be evidently struggling. “But you don’t LOOK sick” is another jarring one that can often prompt the automatic thought of “Oh well I’ll show you what sick is.” Outside appearance can also be deceptive; a diabulimic may present as okay on the outside yet be in acute DKA and in need or emergency assistance. Ultimately, any kind of commentary relating to appearance around someone with an eating disorder should be vetoed wherever possible. Positive or negative, we can take it the wrong way.
3. To a type 1 diabetic with an eating disorder: “Oh wow I could NEVER inject myself.” See the thing is, we sort of die if we don’t and we are trying to avoid that option. “My uncle/great grandfather is diabetic too but he doesn’t have to jab himself.” Yeah, wrong type. Please read a book if you care about me. “Did you become diabetic from eating too much sugar?” “Are you allowed to eat that?!” Just NOPE NOPE NOPE. Especially if you know someone also has an eating disorder. Just NOPE. Educate yourself, please.
4. “You talk about your illness too much; you need to not be so obsessed.” Funny that, see imagine you have this thing on your back every second of every single day, it’s sort of hard to ignore. Don’t stigmatise something that many people with diabetes and eating disorders have struggled to accept and acknowledge. Let us talk, it helps and is far better than denying it exists. Living with this constantly gives us the right to moan and rant and shout if we damn want to.
5. “Wow that’s a huge dinner.” “Ooh that looks like a nice treat!” “Glad to see your appetite is back” I have to say, this often seems to be a dad thing. A stereotypical male that is clueless about nutritional content and thinks the four pork pies he just finished were fewer calories than your sparse meal. We might have a huge plate of salad, yeah lots of leaves, some protein. Or okay we could actually be binging, but we are cringing inside already and it’s too painful acknowledge what it looks like through someone else’s eyes. As with the point about body comments, just refrain from commenting on our food unless we specifically ask for your help or guidance, that has to come from us. Don’t be the food police, as it can cause us to want to isolate even more and protect the disorder, as twisted as that sounds.
6. “Please eat, for me? What did I do wrong? Why are you doing this to me?” This one is a hard one, often from a parent that feels helpless. Personally, the hardest part of being ill has been the hurt it has caused to my loved ones. But it is not about you. Regardless of any relevant cause factors, it comes down to the way WE react. To suggest we would do this to ourselves to spite another person can be painful when most people with eating disorders only want to hurt themselves. It is a mental disorder and rational thought is completely compromised. It can be so powerful that you just don’t realise it’s pulling the strings, and that the control you believed you had was actually your eating disorder playing puppet master.
7. “You just need a good burger/sandwich/slice of cake in you!" (Worse if followed by ‘love’ ‘dear’ ‘darling’) Clearly unhelpful. Eating disorders are not just stubbornness or forgetting to have breakfast in the morning. Often someone that is struggling a lot will find it a huge challenge to eat in public, and that’s not to mention the effort someone with type 1 diabetes needs to do to determine carbohydrates and insulin doses. Sometimes it doesn’t feel worth it, but we shouldn’t have to put on a show to satisfy someone else if it results in us becoming distressed. Let us be.
8. “If you think you are fat you must think I am obese!” Again, anorexia, bulimia, BED, and ED-DMT1/Diabulimia, are all specific to the sufferer. Body dysmorphia is very commonly linked and an eating disorder sufferer may see a different image in the mirror to what others around them can see. We are the exception to the rule. Additionally with Diabulimia the fact that eating disorders are NOT about weight is even clearer HBA1C levels being a far more accurate risk indicator. People with Diabulimia will often have huge fluctuations in weight as they manipulate insulin levels and so this cannot be used to determine how well or unwell someone is,
9. “I wish I could lose weight that quickly!” “I wish I was as thin as you” “god what’s your secret?!” Ha, you really want to know? All completely inappropriate if someone doesn’t know the circumstances being someone’s weight or behaviours. Another that links to the first is “god I’d love to be able to eat anything I wanted and lose weight.” Oh well you can gladly have my diabetes and diabulimia if you want! No refund policy though. Take the ketone breath, fluttering heart and constant thrush with you too.
10. Being told of the damage we are doing to ourselves is simply patronising. We aren’t stupid and nothing will shock us. We know all about the blindness and amputation risk thanks. It’s not lack of intelligence that causes a person with an eating disorder to neglect their health needs. Similarly: “This could kill you, you know?” We sort of do but right now we are more focused on being thin and/or self-destructing.
11. Last but not least and in my opinion the most grating of them all “You do realise that men like a bit of meat on their bones!” Righhht, because I am doing this to myself to snare a man, damn got that on wrong then. Again, ketone breath isn’t much of a turn on. Oh better start eating again if I want to be pretty for boys. I don’t quite understand how this one seems to crop up so often. EATING DISORDERS ARE NOT ABOUT VANITY. If they were then I am definitely going about it the wrong way as I look like crap. Maybe I’ll just tell Mum (see this one seems like a mum thing) that oh well, that’s it then, may as well become a lesbian and join the circus instead.
By Claire Kearns.